Epilepsy audit report
Epilepsy is one of the oldest known conditions and also one of the most common, affecting an estimated 2% of the population. It is characterised by usually unprovoked, clinically discernible events known as seizures, whereby there is synchronous and excessive discharge from collections of neurones (nerve cells) in the cerebral cortex of the brain. These seizures vary greatly in both duration and nature, depending on where they originate as well as the speed and extent of their spread.
Classification
Defining seizures is a difficult task and is often done in accordance with the International Seizure Classification Scheme, as defined by the International League Against Epilepsy in 1981 and 1989. These criteria predate any current imaging or diagnostic techniques and often represent the clinician’s primary source of guidance. The classifications have been recently revised and updated regarding the mode of seizure onset and the classification, the possible categories of causes of epilepsy, the definition of epilepsy syndromes, and other influencing factors.
The key to the revised criteria is the distinction between epilepsy syndromes and disease states. It is now understood that several specific epilepsy syndromes exist, of which each has distinct underlying mechanisms and electro-clinical characteristics. These syndromes are classified according to the stage of life in which they occur, namely, in neonates, infants, children, adolescents, adults or those which are not age-specific. This is known as syndromic diagnosis and is largely due to genetic, developmental or severely extreme environmental factors.
Many epilepsies, however, cannot be categorised as fitting with a syndrome and, in 2006, a more detailed classification list of the different seizures was compiled; individually discussed below. These are divided into those of a focal and generalised nature but there can be overlap between the different categories.
Treatment guidelines for England and Wales are in accordance with those issued by the National Institute of Clinical Excellence in 2004 and were updated in January 2012.
Defining seizures is a difficult task and is often done in accordance with the International Seizure Classification Scheme, as defined by the International League Against Epilepsy in 1981 and 1989. These criteria predate any current imaging or diagnostic techniques and often represent the clinician’s primary source of guidance. The classifications have been recently revised and updated regarding the mode of seizure onset and the classification, the possible categories of causes of epilepsy, the definition of epilepsy syndromes, and other influencing factors.
The key to the revised criteria is the distinction between epilepsy syndromes and disease states. It is now understood that several specific epilepsy syndromes exist, of which each has distinct underlying mechanisms and electro-clinical characteristics. These syndromes are classified according to the stage of life in which they occur, namely, in neonates, infants, children, adolescents, adults or those which are not age-specific. This is known as syndromic diagnosis and is largely due to genetic, developmental or severely extreme environmental factors.
Many epilepsies, however, cannot be categorised as fitting with a syndrome and, in 2006, a more detailed classification list of the different seizures was compiled; individually discussed below. These are divided into those of a focal and generalised nature but there can be overlap between the different categories.
Treatment guidelines for England and Wales are in accordance with those issued by the National Institute of Clinical Excellence in 2004 and were updated in January 2012.
Types of epilepsy
Defining and diagnosing a specific form of epilepsy in a presenting patient is usually a difficult task, since many symptoms overlap and there are huge individual variations in the way epilepsy affects someone. It is therefore easier to analyse the condition in terms of the type of seizure suffered by the patient.
The first main group of seizures is partial seizures. These arise from a localised and specific cortical region and most commonly arise from the temporal lobe of the brain in approximately 60% of people. The frontal lobe is the origin in the majority of other patients. Simple partial seizures are those where the actual neuronal discharge is localised and consciousness is fully preserved. The seizure is often very brief and the individual may feel the stiffening of certain muscle groups. Complex partial seizures mimic simple complex ones yet, crucially, they involve some impairment or loss of consciousness and amnesia of the event. Simple partial seizures commonly progress to become complex.
Particular characteristics of seizures in some individuals, but especially with partial seizures, are known as aura. This is where the patient experiences specific somatosensory, hallucinatory and visual phenomena prior to or during a seizure. These symptoms vary greatly and a table of the most common aura is found below. Aura can also include certain autonomic symptoms such as sweating, flushing and vomiting. Approximately half of all epileptic patients seen by Dr Cockerell report having aura at some stage.
Defining and diagnosing a specific form of epilepsy in a presenting patient is usually a difficult task, since many symptoms overlap and there are huge individual variations in the way epilepsy affects someone. It is therefore easier to analyse the condition in terms of the type of seizure suffered by the patient.
The first main group of seizures is partial seizures. These arise from a localised and specific cortical region and most commonly arise from the temporal lobe of the brain in approximately 60% of people. The frontal lobe is the origin in the majority of other patients. Simple partial seizures are those where the actual neuronal discharge is localised and consciousness is fully preserved. The seizure is often very brief and the individual may feel the stiffening of certain muscle groups. Complex partial seizures mimic simple complex ones yet, crucially, they involve some impairment or loss of consciousness and amnesia of the event. Simple partial seizures commonly progress to become complex.
Particular characteristics of seizures in some individuals, but especially with partial seizures, are known as aura. This is where the patient experiences specific somatosensory, hallucinatory and visual phenomena prior to or during a seizure. These symptoms vary greatly and a table of the most common aura is found below. Aura can also include certain autonomic symptoms such as sweating, flushing and vomiting. Approximately half of all epileptic patients seen by Dr Cockerell report having aura at some stage.
Common presentations of aura in epilepsy
- Nausea and vomiting
- Rising epigastric sensation
- Hallucinations of taste and smell
- Pallor
- Piloerection
- Changes in heart rate
- Intense fear
- Irritability
- Anger
- Dreamy state
- Depersonalisation and derealisation
- Deja-vu
- Vivid recall of childhood memories
- Fidgeting
- Aimless walking
- Lip smacking
- Chewing
- Grimacing
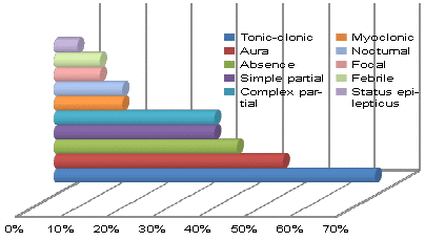
The second main group of seizures is generalised seizures and these are experienced by the vast majority of epilepsy patients. These episodes are bilateral in that they involve both cerebral hemispheres and are thought to arise in the midline before spreading throughout the entire cerebral cortex. The patient always loses consciousness from the outset and usually has some form of motor disturbance due to diffuse hyperexcitability of the membranes in the cortex.
The mildest form of the generalised seizures are known as absences, formerly called petit-mal, which usually begin (and sometimes end) in childhood or teenage years; some patients report absences much later. The patient will suddenly stare into space and blank out for a few seconds, whereby there will often be twitching of the eyelids and/or other sporadic muscles. The episode is commonly interpreted by others as “daydreaming” however the patient will have no recognition or recollection of the event. As such, they can occur numerous times in a day and can disturb school performance in children. There may be slight hyperventilation preceding an absence. Absences are easily detected on an EEG trace, with a characteristic pattern of 3Hz per second spike-and-wave discharges.
Focal motor or Jacksonian seizures occur when the partial electrical discharge originates in the motor cortex and causes jerking movements in the hands, arms, legs, face or a combination of these.
Tonic-clonic epilepsy (grand-mal) represents the largest group of patients and is the most common and recognisable in adults. General malaise with or without aura will normally precipitate an attack although there is often no clear warning. Some patients will find that certain trigger factors, commonly alcohol, sleep deprivation or severe stress, will provoke a seizure and these should clearly be avoided.
The tonic phase occurs initially whereby the person becomes totally rigid for approximately 10-40 seconds and there is a tonic, sustained contraction of all the muscles. This causes the patient to let out a cry before falling directly to the floor. Injuries upon falling, such as lacerations or bruising, are unfortunately common. There is constriction of the pharyngeal and respiratory muscles, leading to a forced violent expiration and possible brief apnoea and cyanosis. The patient may suffer from urinary/faecal incontinence and rigidity may cause them to bite their tongue.
The clonic phase follows, with strong rhythmic contractions of the limbs leading to the convulsive appearance. There may be some degree of frothing at the mouth, slow breathing and a raised heart rate and the clonic phase can last up to several minutes. The final stage is known as postictal and involves the patients regaining consciousness but remaining in a comatose-like state, suffering from extreme drowsiness, lethargy, confusion and amnesia of the episode. A headache may persist following the seizure and it is important to rest and recover sufficiently.
Febrile seizures usually occur in children between 6 months and 6 years old and are associated with a raised core body temperature above 38°C common with many childhood infections. They are commonly isolated events and not a predictor of epilepsy in adulthood but rarely they can persist.
Juvenile Myoclonic Epilepsy (JME) occurs in 4-10% of epileptics but is underdiagnosed. Beginning between the ages of 8 and 18, it is a syndrome that involves a combination of absences, bilateral or unilateral myoclonic arm jerks and possibly tonic-clonic seizures, which usually occur soon after waking. It is important to note that many seizures of all types are nocturnal and can occur during sleep as well as during the day.
Status epilepticus is a medical emergency whereby the patient experiences successive tonic-clonic seizures without regaining consciousness in between. Once the 30-minute threshold is passed, the patient requires emergency intravenous treatment with diazepam or lorazepam to initiate recovery and terminate the seizures.
The mildest form of the generalised seizures are known as absences, formerly called petit-mal, which usually begin (and sometimes end) in childhood or teenage years; some patients report absences much later. The patient will suddenly stare into space and blank out for a few seconds, whereby there will often be twitching of the eyelids and/or other sporadic muscles. The episode is commonly interpreted by others as “daydreaming” however the patient will have no recognition or recollection of the event. As such, they can occur numerous times in a day and can disturb school performance in children. There may be slight hyperventilation preceding an absence. Absences are easily detected on an EEG trace, with a characteristic pattern of 3Hz per second spike-and-wave discharges.
Focal motor or Jacksonian seizures occur when the partial electrical discharge originates in the motor cortex and causes jerking movements in the hands, arms, legs, face or a combination of these.
Tonic-clonic epilepsy (grand-mal) represents the largest group of patients and is the most common and recognisable in adults. General malaise with or without aura will normally precipitate an attack although there is often no clear warning. Some patients will find that certain trigger factors, commonly alcohol, sleep deprivation or severe stress, will provoke a seizure and these should clearly be avoided.
The tonic phase occurs initially whereby the person becomes totally rigid for approximately 10-40 seconds and there is a tonic, sustained contraction of all the muscles. This causes the patient to let out a cry before falling directly to the floor. Injuries upon falling, such as lacerations or bruising, are unfortunately common. There is constriction of the pharyngeal and respiratory muscles, leading to a forced violent expiration and possible brief apnoea and cyanosis. The patient may suffer from urinary/faecal incontinence and rigidity may cause them to bite their tongue.
The clonic phase follows, with strong rhythmic contractions of the limbs leading to the convulsive appearance. There may be some degree of frothing at the mouth, slow breathing and a raised heart rate and the clonic phase can last up to several minutes. The final stage is known as postictal and involves the patients regaining consciousness but remaining in a comatose-like state, suffering from extreme drowsiness, lethargy, confusion and amnesia of the episode. A headache may persist following the seizure and it is important to rest and recover sufficiently.
Febrile seizures usually occur in children between 6 months and 6 years old and are associated with a raised core body temperature above 38°C common with many childhood infections. They are commonly isolated events and not a predictor of epilepsy in adulthood but rarely they can persist.
Juvenile Myoclonic Epilepsy (JME) occurs in 4-10% of epileptics but is underdiagnosed. Beginning between the ages of 8 and 18, it is a syndrome that involves a combination of absences, bilateral or unilateral myoclonic arm jerks and possibly tonic-clonic seizures, which usually occur soon after waking. It is important to note that many seizures of all types are nocturnal and can occur during sleep as well as during the day.
Status epilepticus is a medical emergency whereby the patient experiences successive tonic-clonic seizures without regaining consciousness in between. Once the 30-minute threshold is passed, the patient requires emergency intravenous treatment with diazepam or lorazepam to initiate recovery and terminate the seizures.
Causes
Epilepsy equally affects men and women. The actual underlying cause of the condition is largely unknown and an estimated 60-75% of patients have no clear cause, known as being cryptogenic. The following represent some of the known causes however:
- Head trauma and brain injury (post-traumatic epilepsy)
- Infection, particularly meningitis
- Vascular – haemorrhages and arteriovenous malformations
- Severe and chronic alcohol abuse
- Drugs
- Fever
Whilst the temporal lobe is the most common site of origin, different epileptic symptoms can be attributed to abnormal discharges in different parts of the brain – notably the hippocampus and primary motor cortex. Epileptic neuronal electrical discharge is completely erratic and becomes repetitive, unregulated and unrestricted, with the ability to spread rapidly. Inhibitory mechanisms within the nervous system become overwhelmed and fail to prevent this spread. This results in what is termed “high voltage spike and wave activity”.
In epilepsy, there is thought to be a low seizure threshold, whereby particular groups of neurones have a tendency to become easily hyperexcitable and/or have insufficient inhibitory mechanisms. This makes such patients more prone to seizure than the general population.
The imbalance between excitatory and inhibitory neurones is key to the condition and is thought to involve reduced levels of GABA, an inhibitory neurotransmitter, and raised glutamate, an excitatory neurotransmitter. More recently, the loss of a specialised regulatory cell type known as a chandelier cell is thought to be involved in the pathology of epilepsy.
Diagnosis
Dr Cockerell employs three main methods of diagnosis when assessing a patient. Initially, he takes a detailed medical history, particularly to determine the type of seizure suffered. This may encompass eyewitness descriptions of any event and will usually be accompanied by a neurological physical examination.
The next method is an MRI scan, which is the investigation of choice and is crucial for all epileptic patients, specifically in identifying any abnormalities which would contribute to or cause a seizure.
Thirdly, an electroencephalogram (EEG) involves electrodes being attached to the head to determine (abnormal) electricity activity in the brain. This may be performed whilst the patient is at rest, during sleep or via ambulatory monitoring over an extended period of time and the presence of any spikes, sharp waves or 3Hz spike-wave complexes will be noted. It is important to note however that the EEG is not completely sensitive and a minority of patients will have epilepsy but also a completely normal EEG reading. For this reason, it may be necessary to have repeat EEGs to aid diagnosis.
Dr Cockerell often utilises a specialised form of EEG known as video-telemetry which can more accurately pinpoint the location of seizure origin particularly during an ictal period. It is performed over 24-48 hours and combines EEG readings with imaging techniques.
Treatment
The aim of any treatment of epilepsy is obviously to stop and control the patient from suffering seizures and this can be a complex and lengthy process, with huge variation between individuals. Pharmacological therapy is the main and most effective course of action, although, as mentioned, trigger avoidance is a key prerequisite to such treatment.
Anticonvulsant drugs are varied in their mechanisms of action and it is not entirely known how and why certain drugs treat epilepsy in certain patients and not in others. There is often a “trial and error” approach, whereby the dose and/or drug may need to be changed until a suitable therapy is tailored to achieve good control in that individual without causing (significant) side effects. A balance between efficacy and toxicity is key, as in all aspects of medicine. Treatment will often involve the patient taking one or more drugs for a prolonged period of time. Compliance is vital in reducing the risk and incidence of seizures and it is important that drug regimens agreed with Dr Cockerell are understood and followed to prevent relapse.
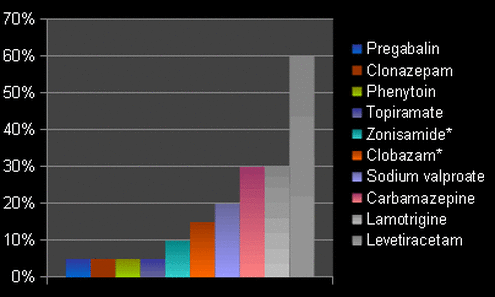
In principle, the classical antiepileptic drugs work to enhance the inhibitory role of GABA or to inhibit the function of voltage-dependent sodium channels, which are implicated in seizure generation. In line with current guidance, Dr Cockerell uses one or more of the following three classic antiepileptic drugs as first-line therapy for treatment of tonic-clonic, simple partial and complex partial seizures.
Other choices include:
New antiepileptic drugs
There have been great advancements in the development of new drugs to treat epilepsy which have varied mechanisms of action and provide a greater choice to both clinician and patient. These are referred to as the “newer” antiepileptic drugs.
Other newer antiepileptics include:
Doses of all drugs are titrated, in that the dose is increased very gradually over weeks or months to the maximum dose in order to reduce the risk of side effects. Non-pharmacological treatment such as surgery is uncommon and restricted to a small number of patients with very specific symptoms and conditions.
Future drugs in development
More potential antiepileptic drugs are being investigated in current research. These include Brivaracetam (related to Levetiracetam but with a far higher affinity); Carisbamate, similar to an existing, rarely used drug, but with fewer side effects; Ganaxolone, which directly activates the subunits that make up the GABA A receptors; and Tonabersat, an inhibitor of neuronal gap junctions.
- Carbamazepine (Tegretol™) – affects membrane excitability by binding to the inner pore of sodium channels. It is one of the most widely used drugs in epilepsy and generally well tolerated by patients with a low relative incidence of side effects, but it can cause dizziness, headache, nausea, some double vision and occasionally skin rashes. Dr Cockerell prescribes Carbamazepine in doses ranging from 600-1500mg per day.
- Sodium valproate (Epilim™) – an inhibitor of the GABA transaminase enzyme, valproate works via a range of mechanisms on both sodium and calcium channels. It has a particularly low incidence of side effects but these can include alopecia, weight gain or gastrointestinal symptoms. The drug is prescribed at 200-2000mg per day.
- Lamotrigine (Lamictal™) – reducing the release of glutamate by its action on sodium channels, lamotrigine can cause rashes, acne, headaches, dizziness and drowsiness but, again, side effects are uncommon. It is given in doses of 50-400mg per day.
Other choices include:
- Ethosuximide – specifically for the treatment of absence seizures, it targets T-type calcium channels.
- Phenytoin – one of the oldest anticonvulsant drugs but used far less today, it has a potent use-dependent blocking action on sodium channels but has a greater risk of side effects.
- Clobazam and clonazepam (Rivotril™) – adjunct therapies and members of the benzodiazepine class used primarily to treat anxiety disorders, they enhance the activity of the GABA receptors.
New antiepileptic drugs
There have been great advancements in the development of new drugs to treat epilepsy which have varied mechanisms of action and provide a greater choice to both clinician and patient. These are referred to as the “newer” antiepileptic drugs.
- Levetiracetam (Keppra™) – Dr Cockerell also prescribes levetiracetam as first-line therapy in the majority of patients. It works by binding to a protein known as SV2A and can cause irritability, drowsiness and dizziness. It is prescribed up to doses of 1500mg/day.
- Retigabine – now licensed for use in the UK, Retigabine represents a novel approach to epilepsy treatment. It activates and opens the KCNQ (Kv7) voltage-gated potassium channel which mediates an “M-current”, a crucial step in the control of neuronal excitability. M-current reductions decrease the hyperexcitability present in epilepsy. These potassium channels are widely distributed in the central nervous system and dorsal horn ganglia and are also thought to be implicated in nociceptive (pain) responses. Retigabine is useful as an adjunctive therapy for partial seizures but is thought also to be a potent inhibitor of acute seizures, possibly where other drugs have failed. Doses are between 600-1200mg/day and side effects of fatigue and dizziness are mild and rare.
- Lacosamide (Vimpat™) – currently licensed as an adjunctive therapy of partial-onset seizures in adults, Lacosamide is also used to treat migraine, fibromyalgia and diabetic neuropathy. It selectively enhances the blockage and inactivation of sodium channels but, uniquely, targets slow (not rapid) inactivation processes. Given at 200-600mg/day by tablet, syrup or intravenous infusion, Lacosamide has the potential to protect against a variety of seizure types and can prevent status epilepticus. Research has demonstrated good tolerance and very few side effects.
Other newer antiepileptics include:
- Gabapentin and pregabalin – calcium-channel blockers for partial seizures that are extremely safe
- Zonisamide – originally an antibacterial, it is thought to act on both sodium and T-type calcium channels. It can cause tiredness, weight loss and loss of appetite
- Vigabatrin – inhibits the breakdown of GABA by blocking the enzyme GABA transaminase
- Tiagabine - reduces the uptake of GABA by inhibiting the GAT-1 transporter protein in the brain
- Topiramate – varied mechanisms of action on sodium and calcium channels, GABA and AMPA receptors
Doses of all drugs are titrated, in that the dose is increased very gradually over weeks or months to the maximum dose in order to reduce the risk of side effects. Non-pharmacological treatment such as surgery is uncommon and restricted to a small number of patients with very specific symptoms and conditions.
Future drugs in development
More potential antiepileptic drugs are being investigated in current research. These include Brivaracetam (related to Levetiracetam but with a far higher affinity); Carisbamate, similar to an existing, rarely used drug, but with fewer side effects; Ganaxolone, which directly activates the subunits that make up the GABA A receptors; and Tonabersat, an inhibitor of neuronal gap junctions.
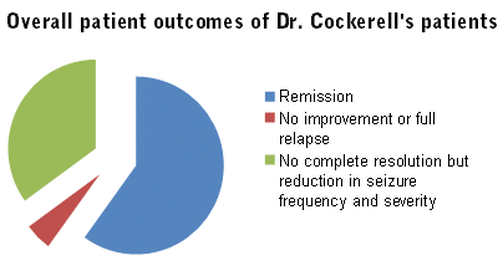
Dr Cockerell has an extremely good success rate in the treatment of epilepsy. The ideal outcome is clearly to achieve remission – control to the point of the patient being seizure-free. This is achieved in approximately 60% of patients he sees. Clearly remission is not always possible, still a further 35% experience a large reduction in symptom severity and frequency. Common clinical practice is only to contemplate drug withdrawal after a substantial period of remission, usually a minimum of two years, although this varies between individuals and is not always possible.
Pregnancy
Pregnancy is a key issue for female epileptics. Many antiepileptic drugs substantially interfere with oral contraceptives and it may be necessary to increase the doses of these to maintain effective cover. Breakthrough bleeding is often a sign of inadequate contraceptive dosage and any such symptoms need to be discussed with Dr Cockerell.
Epilepsy medications bring a higher risk of foetal malformations, notably those of cleft lip/palate and spina bifida. Whilst folic acid supplementation can reduce this risk, the overall aim is to reduce therapy as far as is safe during pregnancy. It must be noted that seizures during pregnancy can also damage the foetus and cause difficulties in labour; therefore issues surrounding pregnancy should be discussed with Dr Cockerell so a suitable treatment decision and regimen can be arranged.
Driving and lifestyle
All epileptic patients are required by law to inform the DVLA of their condition – regardless of the type of seizure suffered. Failure to do so is a criminal offence.
Whilst the patient should initially stop driving immediately, in many instances they can reapply for a licence dependent upon them not having had any seizures while awake in the previous year or on only having had nocturnal seizures for the past three years. This is a decision which the DVLA decides upon and Dr Cockerell can provide appropriate supporting documentation.
Very few lifestyle changes are otherwise required of epileptic patients. In the vast majority of cases, the patient can still partake in most sporting activities and hobbies unless they are particularly risky. Epilepsy similarly does not limit one from the majority of occupations.
Pregnancy is a key issue for female epileptics. Many antiepileptic drugs substantially interfere with oral contraceptives and it may be necessary to increase the doses of these to maintain effective cover. Breakthrough bleeding is often a sign of inadequate contraceptive dosage and any such symptoms need to be discussed with Dr Cockerell.
Epilepsy medications bring a higher risk of foetal malformations, notably those of cleft lip/palate and spina bifida. Whilst folic acid supplementation can reduce this risk, the overall aim is to reduce therapy as far as is safe during pregnancy. It must be noted that seizures during pregnancy can also damage the foetus and cause difficulties in labour; therefore issues surrounding pregnancy should be discussed with Dr Cockerell so a suitable treatment decision and regimen can be arranged.
Driving and lifestyle
All epileptic patients are required by law to inform the DVLA of their condition – regardless of the type of seizure suffered. Failure to do so is a criminal offence.
Whilst the patient should initially stop driving immediately, in many instances they can reapply for a licence dependent upon them not having had any seizures while awake in the previous year or on only having had nocturnal seizures for the past three years. This is a decision which the DVLA decides upon and Dr Cockerell can provide appropriate supporting documentation.
Very few lifestyle changes are otherwise required of epileptic patients. In the vast majority of cases, the patient can still partake in most sporting activities and hobbies unless they are particularly risky. Epilepsy similarly does not limit one from the majority of occupations.
References
- Lindsay KW, Bone I (2004). Neurology & Neurosurgery Illustrated. Churchill Livingstone, 4th Ed.
- Kumar P, Clark M (2005). Clinical Medicine: Chapter 21 – Neurological Disease. Elsevier Saunders, 6th Ed.
- Fowler TJ, Scadding JW (2003). Clinical Neurology: Chapter 15 – Epilepsy and Sleep Disorders by MC Walker and JWAS Sander. Arnold Hodder Publishing, 3rd Ed.
- NHS Choices – Epilepsy. http://www.nhs.uk/Conditions/Epilepsy/Pages/ Accessed on 15 June 2011.
- NICE Guidelines – A Reference Guide. “The epilepsies: diagnosis and management of the epilepsies in adults in primary and secondary care”.
- Fuller G, Manford M (2002). Neurology: An Illustrated Colour Text. Churchill Livingstone, 2nd Ed.
- Rang HP, Dale MM, Ritter JM, Flower RJ, Henderson G (2011). Pharmacology. Elsevier Churchill Livingstone, 7th Ed.
- Macleod S, Appleton RE (2007). The New Antiepileptic Drugs. Arch Dis Child Educ Pract Ed 92: 182-188
- Bialer M, Johannessen SI, Levy RH, Perucca E, Tomson T, White HS (2009). Progress Report on New Antiepileptic Drugs: Summary of the 9th Eilat Conference (Eilat IX). Epilepsy Res. 83: 1-43.
